
Beginning with the Continental Congress authorizing the establishment of a hospital for its army of 20,000 soldiers in 1775, the United States has provided healthcare to its active military members for hundreds of years.
Among the developments before the 20th Century:
- July 1776 - Continental Army Medical Department is established
- Aug. 1842 - Navy Bureau of Medicine and Surgery is established
- May 1862 - Army Medical Museum is established to serve as a center for the collection of specimens for research in military medicine and surgery.

The Air Force Medical Service was founded in 1949 when the U.S. Army and President Harry S. Truman concluded the U.S. Air Force needed its own medical service.

In 1949, the Secretary of Defense established the Office of Medical Services, with a director who had authority to set general policies for the medical services of all three military departments.

In 1951, DOD strengthened the Office of Medical Services and renamed it the Armed Forces Medical Policy Council. The new agency provided coordination of medical policy within the Office of the Secretary of Defense, DOD, other government agencies, and civilian medical and allied health organizations, agencies, and professions.
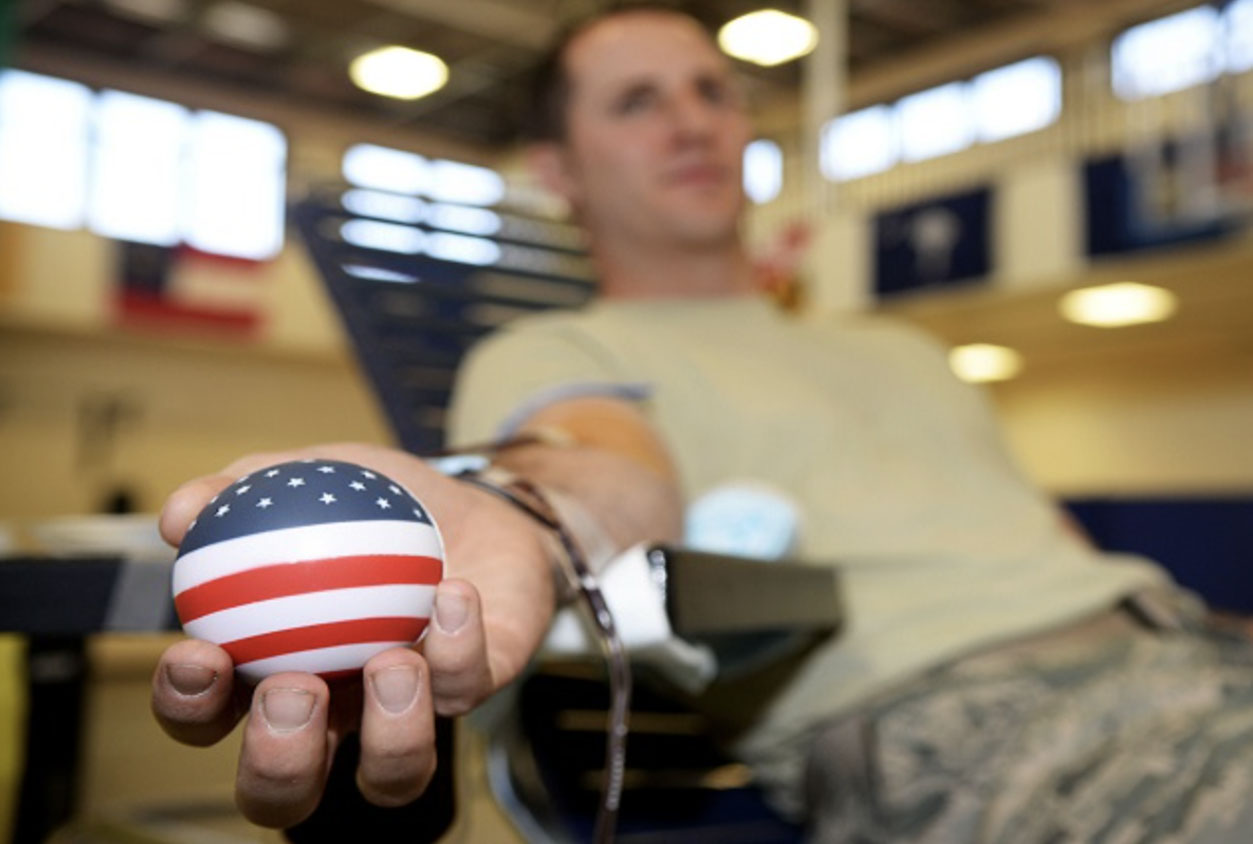
President Harry Truman implemented the ASBP in 1952 as a joint field operating agency, and it became a fully operational blood program in 1962. After the Korean War, ASBP assumed collecting, processing, and transporting blood products for the military community from the American Red Cross. When the Vietnam War started, the ASBP was a distinct program, ready to support the military's blood product needs.

Congress passed the Dependents' Medical Care Act, officially establishing healthcare for active duty family members, retirees, and their family members at military treatment facilities, on a space-available basis.

The Military Medical Supply Agency was conceived to run as manager for wholesale supply of medical and dental material for the three military services, with the Navy serving as its executive agency.

The Wound Data and Munitions Effectiveness Team was established during the Vietnam War. The team included medical and weapons experts who collected data on wounds and injuries sustained by service members during the war. The team's findings were used to improve the design and effectiveness of military weapons and protective gear.

Congress passed the Military Medical Benefits Amendments. Collectively, these acts founded the Civilian Health and Medical Program of the Uniformed Services, known as CHAMPUS. CHAMPUS established a way for DOD to contract with civilian facilities so beneficiaries could receive non-hospital-based services through civilian healthcare plans.

The Defense Department ushered in electronic healthcare documentation with computerized physician order entry. This allowed physicians to record prescribed medications and view alerts for drug allergies or adverse interactions. This innovation marked the beginning of electronic healthcare across military medical departments.

The Composite Healthcare System was the DOD's first health record system to go paperless with electronic order entry. CHCS is also the basis of the Armed Forces Health Longitudinal Technology Application, which focused on delivering a military treatment facility-centric electronic health record that supported computerized physician order entry and integrated outpatient ancillary services.

Many people first heard about telehealth during the COVID-19 pandemic, but did you know telehealth has been around for more than 30 years? In the 1990s, the medical field was exploring how telehealth and telemedicine could enhance medical operational support. This was most notable in 1993, when the U.S. Army first used video-enabled care in Somalia. This care quickly expanded in 1994 and 1995 during operations in the Balkans.
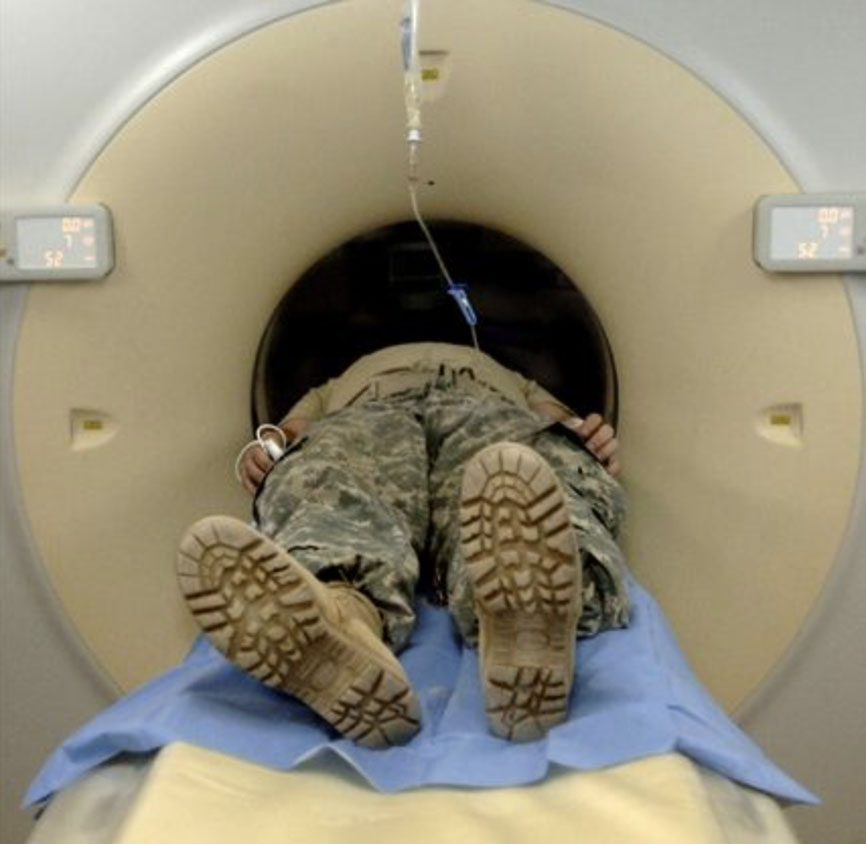
The Defense Department and Department of Veterans Affairs successfully collaborated to form the Defense and Veterans Head Injury Program which was later named the Defense and Veterans Brain Injury Center. The program tracked service members' head and neck injuries, ensured they received the right treatment, studied the treatment outcome, and counseled family members regarding the service members' injuries.

Congress established TRICARE to replace CHAMPUS as the health plan for uniformed service members and their families. TRICARE was launched with three plans: TRICARE Prime, a managed care program similar to an HMO; TRICARE Extra, a preferred provider option; and TRICARE Standard, a fee-for-service model.

The Gulf War Health Center at Walter Reed Army Medical Center was established to care for Gulf War veterans with war-related physical and mental health challenges. In 1999, it became the Deployment Health Clinical Center—one of three DOD centers of excellence for deployment health—along with the Armed Forces Health Surveillance Center and the Naval Health Research Center.

The Combat Casualty Care Research Program was established to drive medical innovation through development of knowledge and materiel solutions for the acute and early management of combat-related trauma, including point-of-injury, en-route, and facility-based care.

Founded on Oct. 31, 1997, the Air Force Research Laboratory leads the discovery, development, and delivery of warfighting technologies for our air, space, and cyber forces. One of the centers is the U.S. Air Force School of Aerospace Medicine, an internationally renowned center for aerospace medical learning, consultation, aerospace medical investigations, and aircrew health assessments. The U.S. Air Force Research Laboratory trains approximately 6,000 students each year.

The end of the Gulf War resulted in the recognition that an electronic health record was needed. President Bill Clinton directed establishment of a new Force Health Protection program. Under his plan, every soldier, sailor, airman, and Marine would have a comprehensive, lifelong medical record.

Defense Secretary William Cohen started reforms to separate elements of the DOD Health Affairs agency's operations and from policy making. Health Affairs policy makers remained housed in the Pentagon, while TRICARE operations and support relocated to Washington, D.C., and Aurora, Colorado. The TRICARE Support Office's priorities included force medical protection, Medicare subvention, which provided alternatives for delivering accessible and quality care to certain veterans, and preventive medicine and wellness issues.

DHAPP was established in 2001 to help contain the global health threat posed by the HIV pandemic. DHAPP’s mission was, and still is, to assist foreign militaries in developing HIV control programs in support of global health security and DOD security cooperation efforts.

In 2004, the Composite Healthcare System II deployed worldwide and was rebranded to the AHLTA. The software improvements focused on upgrading operational availability, speed, provider capabilities, and interoperability between DOD and VA.
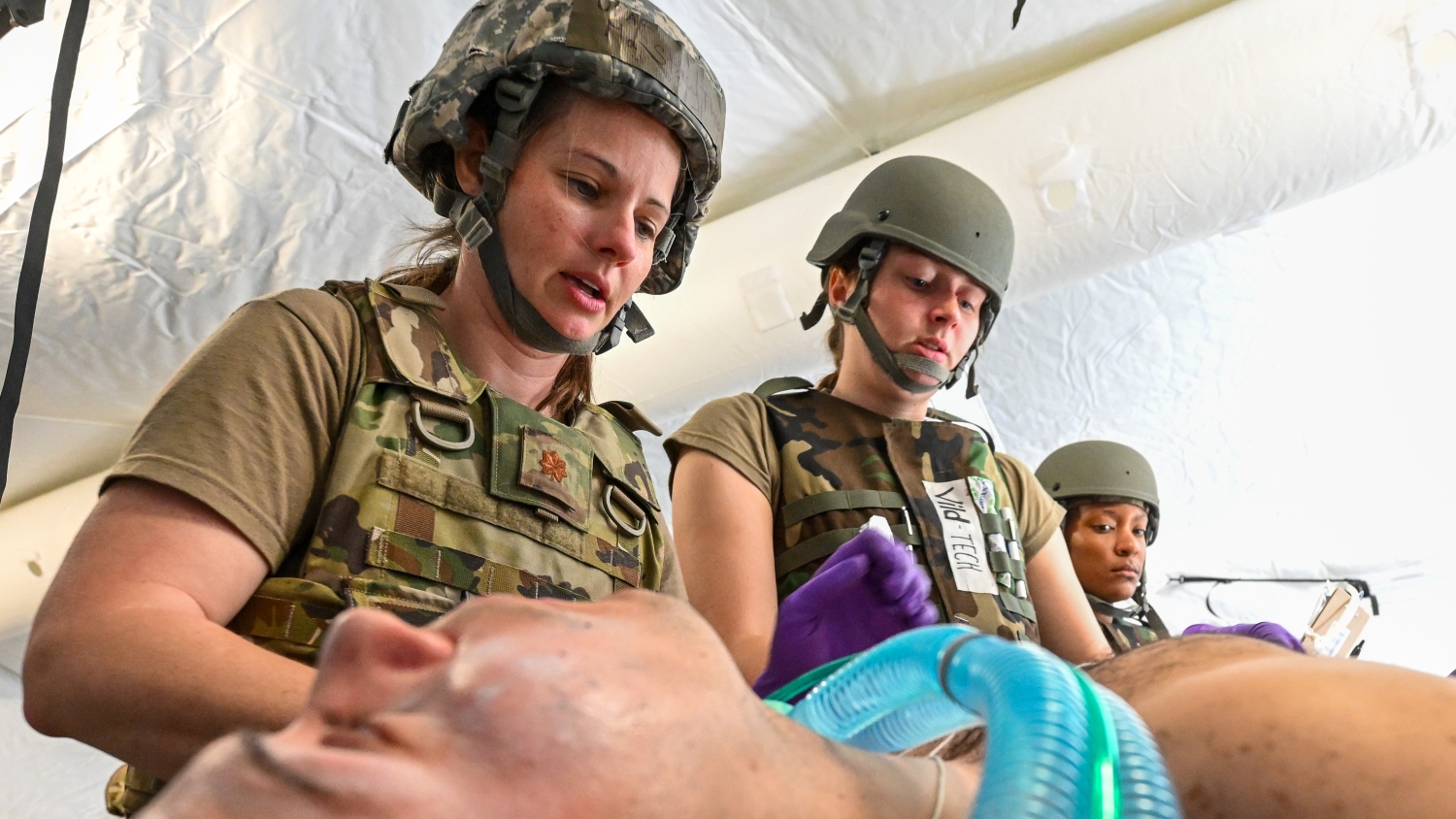
In 2004, the military medical departments were directed to establish a single trauma registry in order to collect and aggregate combat casualty care epidemiology, treatments, and outcomes. This knowledge was essential to understanding the challenges, successes, and failures the military medical corps faced in providing effective and timely care for combat casualties. The Joint Trauma System was established as the agency to build and manage the Joint Trauma Registry.

The Defense Centers of Excellence for Psychological Health and Traumatic Brain Injury began operating in November 2007, and was charged with evaluating, integrating, and promoting psychological health and TBI practices and policies across the services.

The Armed Forces Health Surveillance Center was established in February 2008 to the be central epidemiologic health resource for the U.S. military.

The 2008 National Defense Authorization Act directed DOD to establish a comprehensive plan for programs to prevent, diagnose, treat, and rehabilitate service members with TBI, PTSD, and other mental health conditions.
On March 11, 2013, the Deputy Secretary of Defense issued a memorandum outlining the implementation of MHS governance reform as it was outlined in section 731 of the National Defense Authorization Act for Fiscal Year 2013. While the centerpiece for this reform was the establishment of the DHA as a Combat Support Agency, the memo also established multi-service market areas as geographic areas where at least two military medical hospitals or clinics from different military service branches had overlapping service areas.

On Oct. 1, 2013, DOD established the DHA as a one of eight Combat Support Agencies supporting joint operating forces and Combatant Commands engaged in military operations and to direct the execution of 10 joint shared services: the TRICARE health program; pharmacy operations; health information technology; medical logistics; facility management; research and development; education and training; public health; budget and resource management; and contracting. The TRICARE Management Activity was decommissioned with the establishment of the DHA.

On Sept. 30, 2014, the DHA Public Health Division reached Initial Operating Capability after assuming authorities over three former Army executive agencies, DOD Veterinary Services, the Military Vaccine Healthcare Network and the Armed Forces Health Surveillance Center as public health product lines.

On July 9, 2014, DHA assumed operational management and support of the ASBP and DHAPP. Each program brought a unique combat support capability to the DHA. The ASBP is the official provider of blood products for the U.S. Armed Forces. The DHAPP executes worldwide HIV/AIDS prevention, care, and treatment programs.

On Aug. 23, 2015, the National Museum of Health and Medicine joined DHA. The museum spans five collections consisting of about 25 million artifacts, including the bullet that killed President Abraham Lincoln, 5,000 skeletal specimens, 8,000 preserved organs, 12,000 items of medical equipment, an archive of historic medical documents, and more.

In August 2015, the Armed Forces Health Surveillance Center joined DHA and was renamed the Armed Forces Health Surveillance Branch under DHA’s Public Health Division. Today, the Armed Forces Health Surveillance Division is the central epidemiologic health resource for the U.S. military.

The Armed Forces Medical Examiner System has a history dating back to the 1950s and early 1960s, which evolved by the expansion of the Armed Forces Institute of Pathology's field of study that included a forensic pathology registry in 1958. In 1959, the Military Environmental Pathology Division was established, consisting of forensic pathology, aviation medicine, and toxicology. In 1962, the first forensic pathology fellowship in the United States was established. AFMES was formally transferred from MRMC to the DHA on Aug. 31, 2015.

The Defense Department awarded the contract to build the Department's electronic health record, later branded as MHS GENESIS. The deployment of MHS GENESIS began in the Pacific Northwest in 2015 followed by 25 unique waves encompassing military hospitals and clinics in the U.S.. In September 2023, MHS GENESIS began to deploy to military hospitals and clinics in the European and Indo-Pacific regions.

On Oct. 1 2015, DHA achieved full operational capability, two years after the agency was first established.

In fall of 2016, the Office of the Under Secretary of Defense for Personnel and Readiness recommended the DOD "establish the JTS, in its role as the DOD Trauma System as the lead agency for trauma in DOD with authority to establish and assure best-practice trauma care guidelines to the DHA Director, the Services, and the Combatant Commanders.
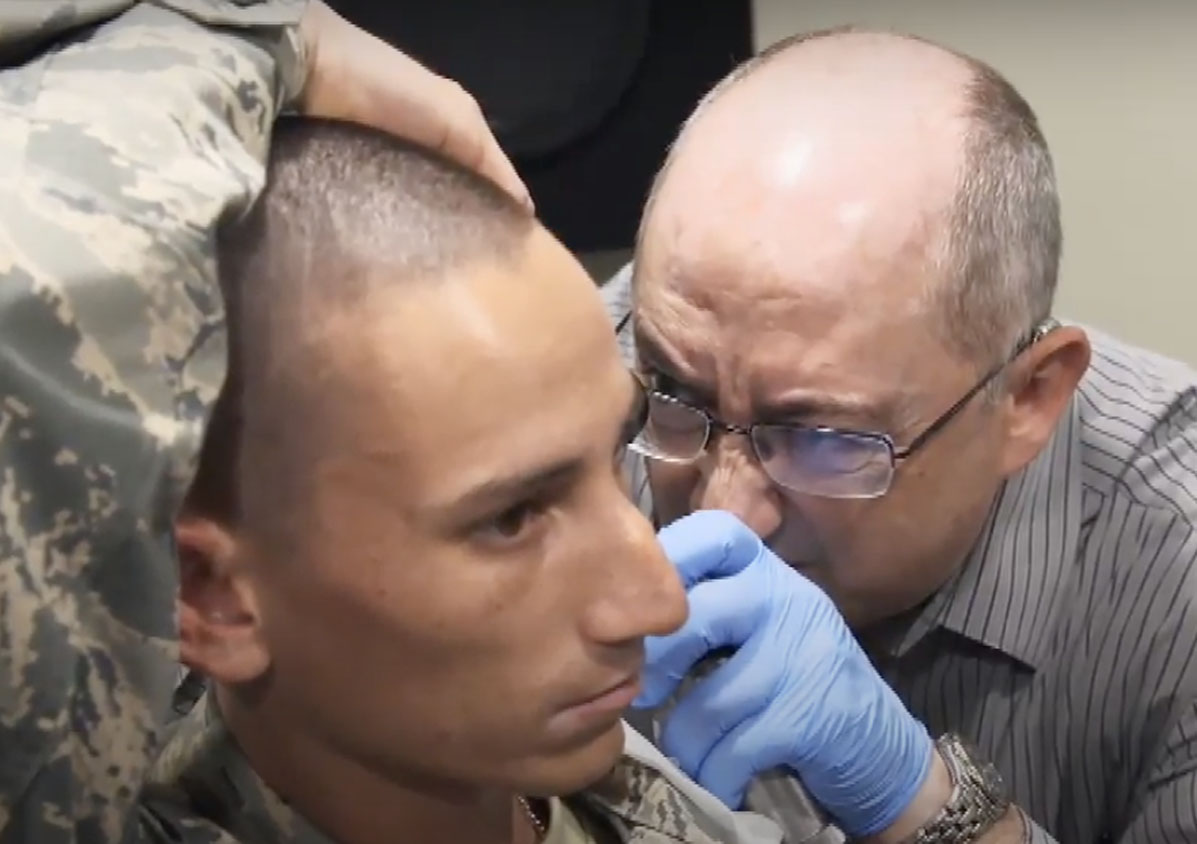
On Dec. 11, 2016, the Hearing Center of Excellence became a part of DHA. The Center focuses on the prevention, diagnosis, mitigation, treatment, and rehabilitation of hearing loss and auditory injury. It also partners with the VA, institutions of higher education, and other mission-minded public and private organizations to advance research and care in hearing loss.
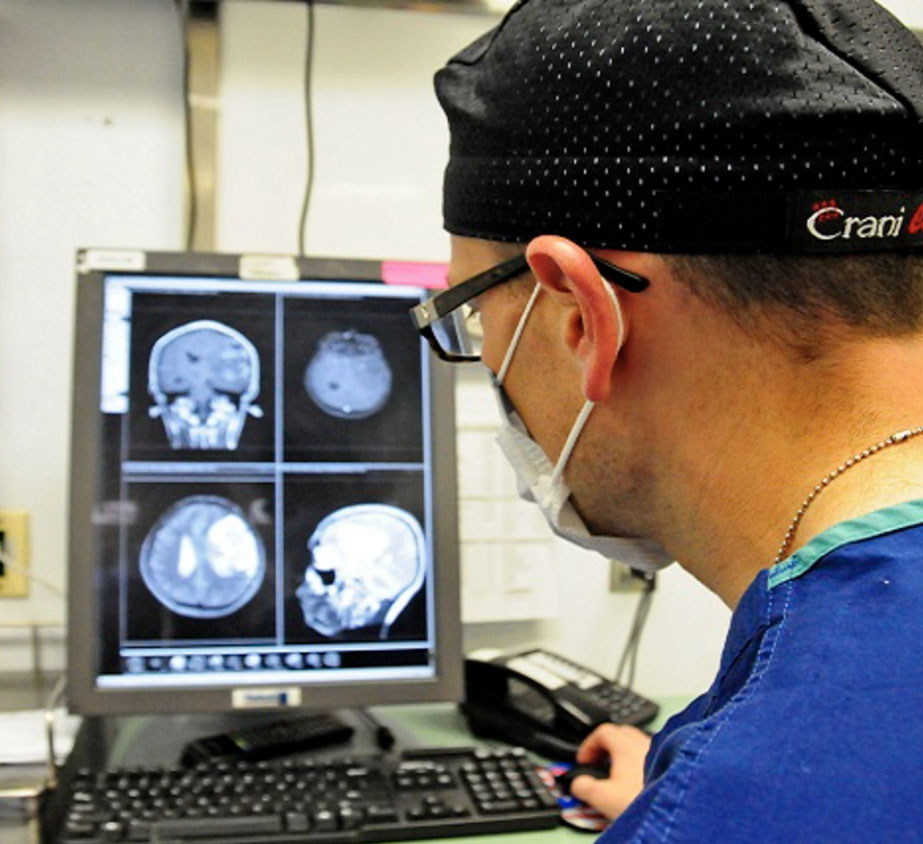
In 2016, the Defense Centers of Excellence for Psychological Health and Traumatic Brain Injury and its centers transitioned to DHA. The Deployment Health Clinical Center officially changed its name to the Psychological Health Center of Excellence to better align with its current mission. The Defense and Veterans Brain Injury Center retained its enduring mission of evaluating, integrating, and promoting TBI practices and policies across the services.

Section 702 of the Fiscal Year 2017 National Defense Authorization Act and subsequent guidance provided by Congress in 2018, 2019, and 2020 directed the Military Health System to reorganize, redefining the roles of the military departments and DHA in the administration and management of military hospitals and clinics.
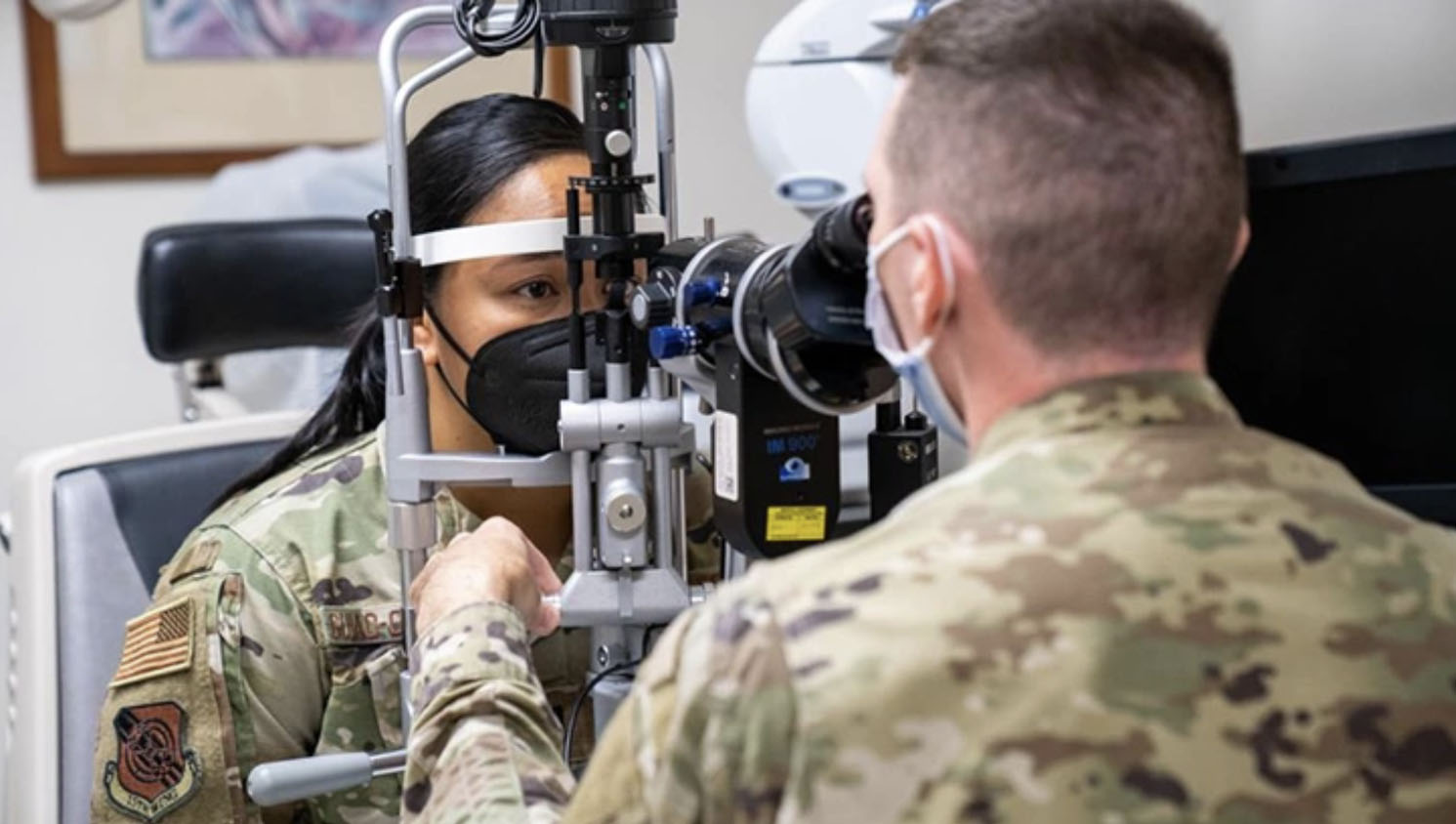
In March 2018, the Vision Center of Excellence joined the DHA family to address the full scope of vision care in the armed forces, including prevention, diagnosis, mitigation, treatment, research, and rehabilitation of military eye injuries and diseases in order to improve vision health, optimize readiness, and enhance quality of life for service members and veterans.

To ensure consistent, high-quality care across the enterprise, all military hospitals and clinics began to follow DHA standardized policies, procedures, and clinical and business practices on Oct. 1, 2018.

On Oct 1, 2019, following requirements set forth in the 2017 NDAA, military hospitals and clinics around the world were re-organized beneath the umbrella of the DHA, further helping to standardize care.
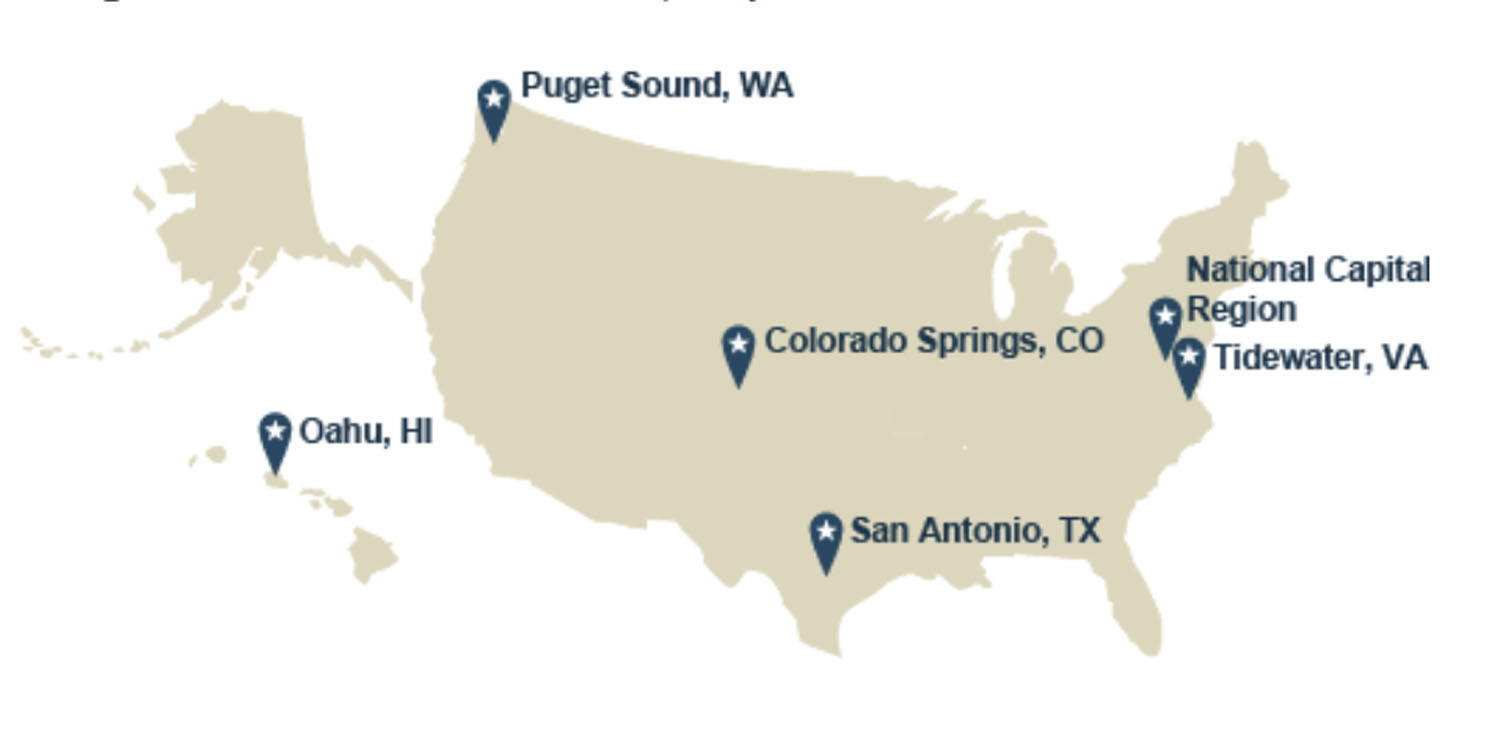
On Jan. 30, 2020, medical facilities were organized into four regions within the United States. These “markets” included hospitals and clinics in the National Capital Region (Washington, D.C., southern Maryland, and northern Virginia), along with Jacksonville, Florida, the Mississippi coast (Biloxi, Gulfport, and Pascagoula), and Central North Carolina (Fayetteville). Following a brief pause during the COVID-19 pandemic, Tidewater became the 5th market to be established on April 19, 2021.

In October 2022, the Army, Navy/Marine Corps, and Air Force moved public health centers and programs to the DHA. The newly established DHA Public Health enterprise supports the Joint Force and the DOD across the globe by combining and integrating the efforts of the service components to enable a healthy ready force that includes our military families and other beneficiaries.

DHA Director Lt. Gen. (Dr.) Ronald Place presided over a ceremony in Germany on Oct. 25, 2022, marking the end of a four-year process to transition more than 700 military medical and dental facilities from the individual military services to DHA.

In 2023, deployment of MHS GENESIS was completed at military hospitals and clinics in the continental U.S. Completed on-time and on-budget, this DOD milestone brought DHA one step closer to providing a standardized and integrated health information system for all beneficiaries.
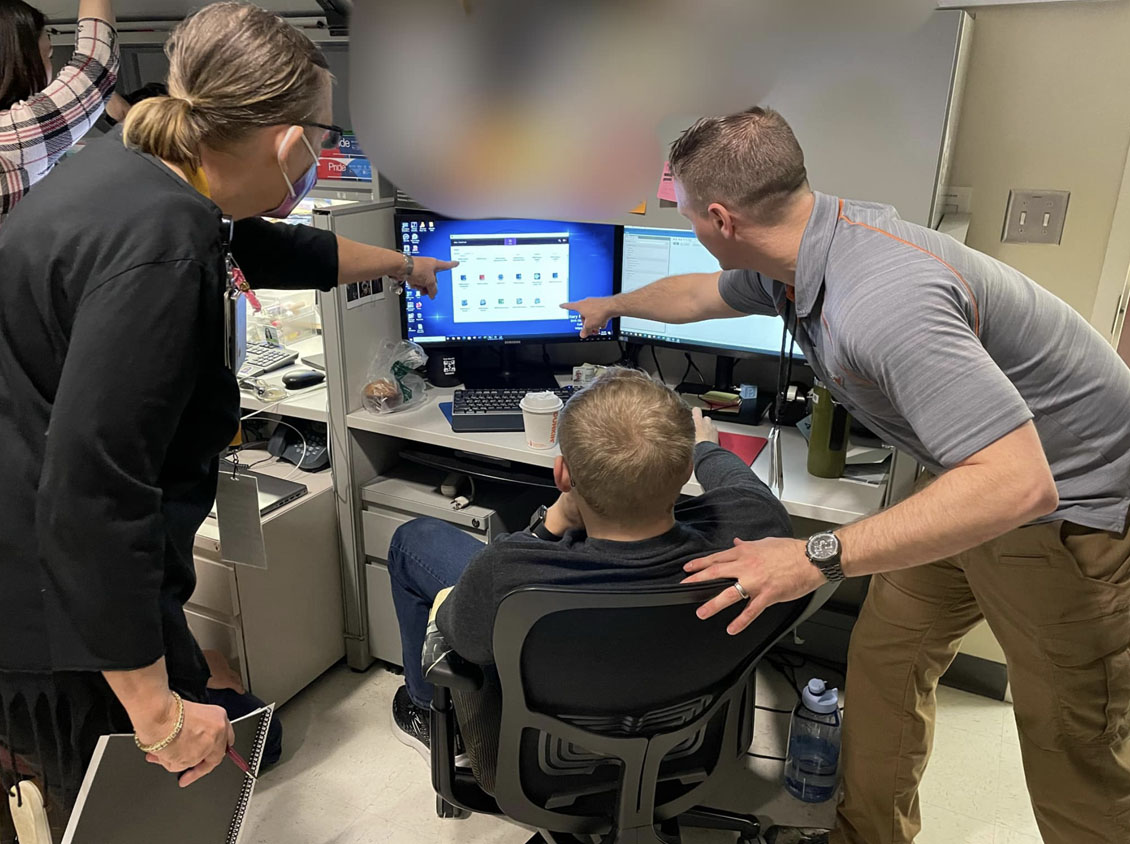
With deployment of MHS GENESIS complete at military hospitals and clinics in the continental United States, sights were set on transitioning overseas. On July. 23, 2023, the deployment wave included overseas military hospitals and clinics at bases in Europe, such as Landstuhl Regional Medical Center in Germany and the Royal Air Force Lakenheath in the United Kingdom.

On Oct. 1, 2023, DHA aligned healthcare administration under nine Defense Health Networks. This change eliminated stand-alone military hospitals and clinics and aligned every facility to a Defense Health Network.

On Mar. 9, 2024, MHS GENESIS deployed to the final DOD military medical treatment facility. The Captain James A. Lovell Federal Healthcare Center and its subordinate clinics in North Chicago, Illinois successfully deployed the new EHR at the first joint Department of Veterans Affairs / DOD facility.
The DHA established the DHA Academy; a consolidation of all staff development and training offerings under a single DHA entity. This initiative supports the DHA strategic initiative – Effective & Timely Acquisition, Development, Retention, and Management of the Agency’s total workforce.
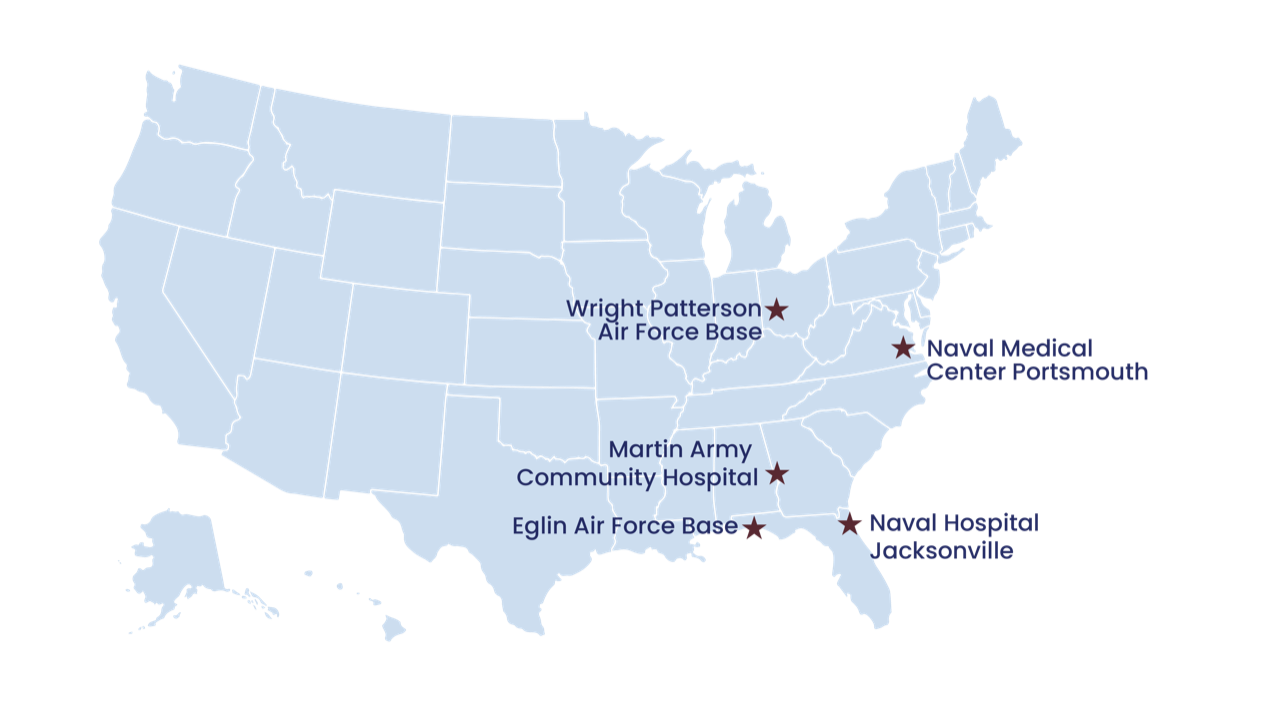
In March 2024, an initiative called “My Military Health” was launched at five venture sites around the nation. The tools were designed offer care that was individualized, accessible, and convenient. My Military Health will be accessible 24/7 by computer and mobile devices, will allow patients to schedule appointments, engage with automated clinical support for medical conditions, and use self-help wellness programs.
The Dec. 2024 launch of www.dha.mil provided the Agency with a standalone platform to share developments and news with stakeholders, provide information for vendors to more easily do business with the Agency, give beneficiaries easily navigable pathways to their own care, and establish an employee hub to highlight the benefits and opportunities available in working for the DHA.

The Defense Health Agency distinguished itself by exceptionally meritorious achievement from Nov. 1, 2020, to June 30, 2021. During this period, the president of the United States and secretary of defense appointed the DHA to develop and execute a vaccination plan to protect 11.3 million eligible personnel worldwide. The first DOD Coronavirus-2019 Vaccine Distribution Plan addressed acquisition, distribution, resourcing, training, administration, reporting, and communications. This is the agency’s fourth Joint Meritorious Unit Award in its nearly 12-year history.

On Oct. 1, 2025, the Defense Suicide Prevention Office transitioned to the DHA. Established in 2011 as part of the Office of the Under Secretary of Defense for Personnel and Readiness, DSPO was created following recommendations from the Defense Health Board Task Force. This transition aligns suicide prevention initiatives within DHA to enhance coordination and support for service members.
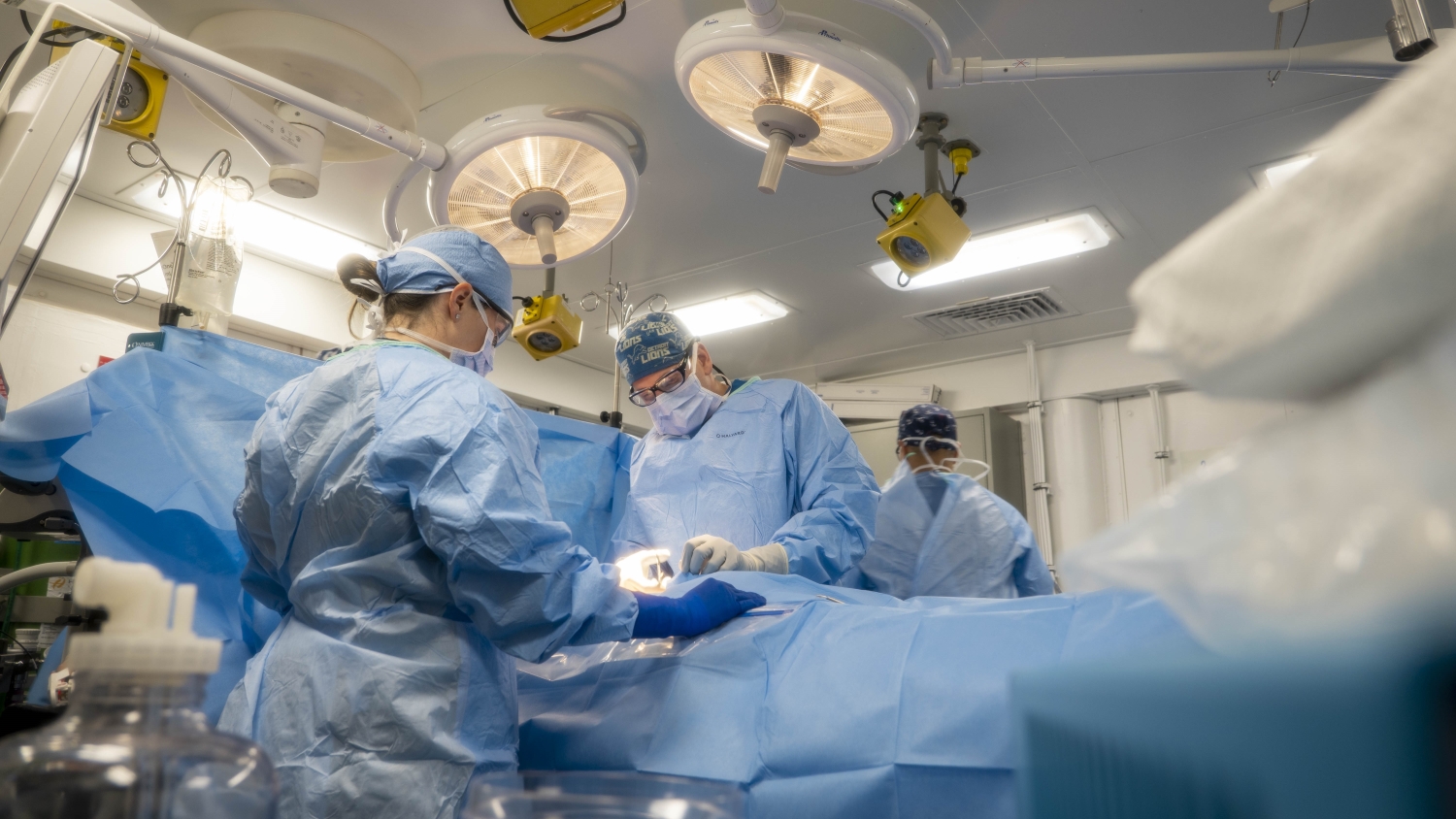
On Oct. 15, 2025, the Defense Health Agency launched an unprecedented privileging process allowing Military Health System providers to retain their clinical privileges when moving between stateside and overseas military hospitals, clinics, and deployed settings. The new enterprise-wide process reduced administrative burdens and addressed long-standing concerns with the privileging process. The new system was an exciting industry innovation that unified all of military medicine for efficient patient care while maintaining appropriate safety mechanisms.



